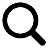Introduction to Laparoscopic Surgery
Laparoscopic surgery, often referred to as minimally invasive surgery, has transformed the landscape of surgical procedures, offering an alternative that significantly reduces patient discomfort and recovery time. This technique involves making small incisions, typically 0.5–1.5 cm, through which a laparoscope (a small camera) and surgical instruments are inserted, allowing surgeons to perform operations with a detailed view of the internal aspects of the abdomen on a monitor.
The advantages of laparoscopic surgery are numerous. It leads to less postoperative pain and scarring, shorter hospital stays, and quicker returns to daily activities when compared to open surgery. The reduced size of incisions not only minimizes the physical impact on patients but also lowers the risk of infection and postoperative complications. These benefits make laparoscopy the preferred approach for many abdominal surgeries, including gallbladder removal, hernia repair, and bariatric surgery, among others.
The decision on the method of entry into the abdominal cavity is pivotal in ensuring the success of a laparoscopic procedure. Two main technologies are currently mainstream: Veress needle technology and Hasson technology.Choosing the appropriate entry technique is influenced by various factors, including the patient's medical history, the presence of scar tissue, and the specific requirements of the surgery. The Veress needle technique is known for its efficiency and the ability to quickly establish pneumoperitoneum (insufflation of the abdomen with gas to create a working space), making it suitable for patients without a history of abdominal surgeries. On the other hand, the Hasson technique, which involves an open approach to gaining access, offers direct visualization of the entry, reducing the risk of injury to abdominal organs. This method is often preferred in cases with anticipated difficulties, such as previous surgeries that may have resulted in adhesions.
The evolution of laparoscopic surgery has been significantly influenced by the development and refinement of these entry techniques. As technology and surgical practices continue to advance, the safety and efficacy of laparoscopic procedures improve, offering patients better outcomes and transforming the standard of surgical care.
Understanding the Veress Needle Technique
The Veress needle technique is a cornerstone in the realm of laparoscopic surgery, enabling the creation of pneumoperitoneum — the essential first step for providing a safe and effective operating space within the abdomen. This method involves the use of a specially designed, spring-loaded needle that ensures safe insertion into the abdominal cavity to insufflate it with gas, typically carbon dioxide. The technique is named after János Veress, a Hungarian physician who invented the needle in the 1930s for initial abdominal insufflation.
Procedure and Mechanism
The process begins with the needle being inserted through a small incision, usually at the umbilicus (navel), where the abdominal wall is thinnest. The needle's unique design features a blunt tip that retracts to expose a sharp point when it encounters resistance, allowing for penetration of the abdominal wall. Once inside the cavity, the blunt tip springs forward to minimize the risk of injuring internal organs. The surgeon then insufflates the abdomen with carbon dioxide, creating a working space by lifting the abdominal wall away from the internal organs. This pneumoperitoneum allows for clear visualization and manipulation of tissues during surgery.
Advantages and Applications
The Veress needle technique is praised for its speed, simplicity, and minimal invasiveness, making it the preferred method for establishing pneumoperitoneum in patients without a history of abdominal surgery. Its design minimizes the risk of injury during entry, and the technique has been refined over the years to enhance safety and efficiency. It is particularly useful in cases where speed is essential, and the surgical site is free of adhesions that could complicate entry.
Considerations and Safety
Despite its advantages, the Veress needle technique requires careful handling to avoid complications such as gas embolism or injury to internal organs. Surgeons must be proficient in its use and aware of the anatomical landmarks and variations in patient anatomy. The choice between the Veress needle and alternative entry techniques, like the Hasson technique, is influenced by the patient's medical history, the presence of scar tissue, and the specific requirements of the surgery being performed.
The Veress needle technique remains a fundamental skill in laparoscopic surgery, embodying the principles of minimally invasive surgery through its design and application. As surgical technology and techniques continue to evolve, the Veress needle serves as a testament to innovation in surgical practice, offering a balance of safety, efficiency, and efficacy.
Exploring the Hasson Technique
The Hasson technique, also known as the open technique, is a critical method for establishing access for laparoscopic surgery that prioritizes safety and control. Developed by Dr. Hasson in the 1970s, this technique involves creating a small incision through which direct visualization and manual placement of the trocar can be achieved, significantly reducing the risk of injury to internal organs. This method is particularly advantageous in patients with a history of abdominal surgery where scar tissue may present an increased risk of complications with blind entry methods.
Procedure and Rationale
The Hasson technique begins with a small incision, typically made below the umbilicus or at the site of previous surgical scars, to access the abdominal cavity directly. The surgeon then carefully dissects through the layers of the abdominal wall under direct vision, ensuring that each layer is clearly identified and safely opened. Once the peritoneum is reached and opened, a blunt trocar is manually inserted into the abdominal cavity. This method allows for the controlled establishment of pneumoperitoneum and placement of the laparoscope, with minimal risk of damaging internal structures.
Advantages and Indications
One of the primary advantages of the Hasson technique is the reduced risk of accidental injury to the abdominal organs or vessels, as the entry is performed under direct visualization. This approach is particularly beneficial for patients with complex medical histories, including previous abdominal surgeries, obesity, or conditions that may complicate blind entry techniques. Moreover, the Hasson technique provides an excellent option for surgeons when encountering difficulties with other entry methods or when the patient's anatomy presents unique challenges.
Considerations and Application
While the Hasson technique offers significant safety benefits, it requires surgical expertise to perform correctly and may take longer than the Veress needle approach. The careful dissection and need for suturing the incision site at the conclusion of the surgery also mean that the technique demands a higher level of skill and meticulous attention to detail.
Despite these considerations, the Hasson technique remains a cornerstone of laparoscopic surgery, embodying the principles of patient safety and surgical precision. Its application across a wide range of laparoscopic procedures underscores its versatility and importance in modern surgical practice.
Comparative Analysis: Veress Needle vs. Hasson Technique
The choice between the Veress needle and the Hasson technique for establishing access in laparoscopic surgery is pivotal, influencing not only the safety and efficiency of the procedure but also its overall success. Both methods have distinct advantages and considerations, making them suitable for different clinical situations. This section provides a comparative analysis, helping surgeons navigate the decision-making process.
Safety and Risk Factors
Veress Needle: Known for its quick and minimally invasive entry, the Veress needle carries a risk of injury to internal organs if not used correctly. However, with proper technique and experience, these risks are minimal.
Hasson Technique: Offers a safer approach by allowing direct visualization of the entry, significantly reducing the potential for accidental organ damage. It is particularly recommended for patients with previous abdominal surgeries where adhesions might be present.
Efficiency and Speed
Veress Needle: Provides a faster route to pneumoperitoneum, making it ideal for situations where time is of the essence. Its simplicity and speed of use are significant advantages in straightforward cases.
Hasson Technique: Requires more time due to the open dissection and suturing of the incision site. However, this investment in time enhances safety and is preferred in complex cases.
Applicability and Indications
Veress Needle: Best suited for patients without a history of abdominal surgery, offering an efficient and less invasive option.
Hasson Technique: Ideal for patients with previous abdominal interventions, obesity, or other factors that increase the risk of complications with blind entry methods.
Expert Recommendations
Experts tend to recommend the Veress needle for routine laparoscopic cases due to its efficiency and minimal invasiveness. In contrast, the Hasson technique is advised when patient history or physical examination suggests a higher risk of complications with blind entry.
Comparison Table: Veress Needle vs. Hasson Technique
| Feature | Veress Needle | Hasson Technique |
| Entry Method | Closed, using a spring-loaded needle | Open, with direct visualization |
| Primary Use | Preferred in patients without previous abdominal surgery | Recommended for patients with prior abdominal surgeries or conditions complicating blind entry |
| Safety | Minimal risk of organ injury with proper technique | Reduced risk of organ injury due to direct visualization |
| Efficiency | Quick establishment of pneumoperitoneum | More time-consuming due to open dissection |
| Complexity | Less complex, requiring specific skill to minimize risks | More complex, requiring careful dissection and suturing |
| Risk of Complications | Potential for organ damage if not correctly positioned | Lower risk of internal organ damage |
| Patient Recovery | Generally faster due to minimal invasiveness | Slightly longer due to the open approach but with enhanced safety |
| Indications | No history of abdominal surgery, less complicated cases | History of abdominal surgery, obesity, or increased risk of adhesions |
Conclusion
Both the Veress needle and Hasson technique have their rightful place in laparoscopic surgery. The choice between them should be guided by the patient's specific circumstances, the surgeon's experience, and the procedural requirements. Understanding the strengths and limitations of each method ensures the highest levels of patient safety and procedural success.
Expert Recommendations and Conclusion
The decision between the Veress needle and Hasson technique is more than a choice of surgical tools; it's a decision that impacts patient safety, surgical efficiency, and overall success of laparoscopic procedures. Both techniques have their place in modern surgery, each with specific advantages that suit different clinical scenarios.
Veress Needle Technique: Its speed and minimal invasiveness make it a valuable option for surgeries where time is critical and the patient has no significant history of abdominal interventions. It demands a high level of skill and understanding to use safely, underscoring the importance of experience and training.
Hasson Technique: This technique shines in its ability to minimize risks through direct visualization during entry. It is particularly beneficial for patients with prior abdominal surgeries or other factors that elevate the risk of complications with blind entry methods. While more time-consuming, its emphasis on safety makes it a preferred choice for complex cases.
Making the Right Choice: The decision on which technique to use should be guided by a thorough evaluation of the patient's medical history, the specific requirements of the surgery, and the surgeon's expertise and comfort with each method. Collaboration and consultation with colleagues can also provide valuable insights, ensuring the chosen method aligns with best practices and patient needs.
Final Thoughts: As laparoscopic surgery continues to evolve, so too will the techniques and technologies that support it. Ongoing research and development are likely to introduce new methods and improvements, further enhancing the safety and effectiveness of minimally invasive surgery. For now, understanding the nuances of the Veress needle and Hasson technique allows surgeons to navigate the complexities of laparoscopic entry with confidence, ensuring the best possible outcomes for their patients.
Related Products


 Français
Français Español
Español Products
Products

 About Us
About Us